RHEUMATOID SHOULDER
Rheumatoid arthritis that affects the shoulder region is a progressive disorder that leads to pain, loss of range ...
Prolapse is a condition in which the organs fall or slide from their place, most exposed being the pelvic organs: uterus, rectum, bladder and small intestine. But a herniated spinal disc is sometimes also called "disc prolapse" and at the level of the heart there may be prolapse of the heart valves (mitral valve) which is a valvar heart disease.
The main cause of prolapse of the pelvic organs is increased pressure at the level of the pelvic floor, most frequently due to pregnancy and childbirth. More precisely, the muscles, ligaments and fascia that support the vagina stretch and weaken during pregnancy, labor and childbirth.
But not all women who have given birth develop pelvic organ prolapse. Some women have very strong supportive muscles, ligaments and fascia of the pelvis. It is also possible for a woman who has not given birth to develop pelvic organ prolapse.

They partly support the uterus, bladder and rectum (the terminal part of the large intestine). A strong pelvic floor provides better support for the pelvic organs, prevents the aggravation of prolapse and relieves the symptoms associated with it.
To strengthen the pelvic floor muscles, Kegel exercises should be regularly practiced. Thus, first of all, the pelvic floor muscles must be localized and in order to locate them we imagine that we are trying to stop the flow of urine and then the Kegel exercises will be performed.
More precisely, the pelvic floor muscles contract for 5 seconds followed by their relaxation for 5 seconds (if it is too difficult, start with the contraction of these muscles for 2 seconds and relax for 3 seconds.) Practice this gradually until you succeeded to hold a contraction for 10 seconds followed by relaxation for 10 seconds.
At least 3 sets of 10 repetitions will be performed daily. Once learned, Kegel exercises can be practiced discreetly almost anytime and anywhere, either at the office or at home.
It occurs when the muscles and ligaments of the pelvic floor stretch, weaken and no longer provide enough support to the uterus. As a result, the uterus slides down or exits the vagina.
Uterine prolapse can occur in women of any age but it affects more frequently postmenopausal women who have had one or more natural births.

Often, the signs and symptoms are less disturbing in the morning and worsen throughout the day. Among them we mention:
➢ feeling of heaviness in the pelvis or pulling down
➢ sensation of tissue coming out of the vagina
➢ urinary problems such as leakage of urine (incontinence) or retention of urine
➢ intestinal peristalsis (constipation) problems
➢ sexual problems due to weakening of the vaginal tissue tone
Treatment depends on the severity of uterine prolapse.
If the symptoms are mild, self-care is sufficient, both in keeping the symptoms under control and in preventing the worsening of the prolapse. Self-care measures include:
➢ performing Kegel exercises to strengthen pelvic muscles
➢ weight loss
➢ treating constipation.
A vaginal pessary is a plastic, silicone or rubber device that is inserted into the vagina to support tissues. The pessary should be removed regularly for cleaning.
Depending on the severity of the prolapse, the surgical intervention consists either in the restoration of the weakened pelvic tissues or in the removal of the uterus (hysterectomy).
Rectal prolapse occurs when a part of the rectum (the terminal part of the digestive tract) slides outside the anus (the muscular opening at the end of the digestive tract.
Although rectal prolapse can cause discomfort, it is rarely a medical emergency.
Rectal prolapse can sometimes be treated with suppositories and other medications, but surgery is usually necessary to treat it.
The cause of rectal prolapse is unclear, women over 50 years of age being more exposed. Although it has often been associated with childbirth, over 2/3 of women with rectal prolapse have no children.

Most commonly, a reddish mass is observed coming out of the anus during an intestinal strain movement. This mass may slide back inside the anus or remain outside it.
Other symptoms may include:
➢ Inability to control intestinal transit (fecal incontinence)
➢ Constipation or diarrhea
➢ Outflow of blood or mucus from the rectum
Treatment for rectal prolapse usually involves surgery through several different surgical methods.
The doctor will choose the best surgical approach taking into account age, physical condition and bowel function.

The bladder is an empty organ located in the pelvis with the function of storing urine.
In women, the front wall of the vagina supports the bladder. This wall can weaken with age or childbirth and if it deteriorates enough, the bladder can prolapse, which means that it is no longer sustained and descends into the vagina.
This can trigger problems such as discomfort and urinary incontinence (urine leakage) caused by sneezing, coughing or exertion.
Prolapsed bladders (also called cystocele or fallen bladders) are divided into 4 degrees depending on how far the bladder descends into the vagina, namely:
➢ 1st degree (mild): Only a small part of the bladder descends into the vagina.
➢ 2nd degree (moderate): The bladder descends enough to be able to reach the opening of the vagina.
➢ 3rd degree (severe): The bladder exits the body through the vaginal opening.
➢ 4th degree (complete): The entire bladder protrudes completely outside the vagina; it is usually associated with other forms of pelvic organ prolapse.
Prolapsed bladders are commonly associated with menopause. Before menopause, estrogen helps keep the muscles inside and around the vagina strong. After menopause because not that much estrogen is secreted, the muscles tend to lose weight.
But natural childbirth remains the most common cause of a prolapsed bladder due to stress on the vaginal tissues and muscles that support the bladder in women.
Other causes that lead to bladder prolapse are lifting heavy objects, bowel tension movements, chronic cough or long-term constipation.

The first symptom usually noticed by women with prolapsed bladder is the presence of tissue in the vagina that many women describe as something that feels like a ball.
Other symptoms of a prolapsed bladder include:
➢ Discomfort or pain in the pelvis
➢ Tissue coming out of the vagina
➢ Difficulty urinating
➢ Sensation of incomplete emptying of the bladder
➢ Urinary stress incontinence (leakage of urine during sneezing, coughing or physical exertion)
➢ More frequent infections of the bladder
➢ Painful sexual intercourse (dyspareunia)
➢ Low back pain
Any woman who notices symptoms of a prolapsed bladder should go to the doctor, there are several treatments to treat a prolapsed bladder.
Thus, when there is only a small part of the bladder lowered into the vagina (1st degree prolapsed bladder) that does not cause pain or discomfort, usually the specialist doctor recommends avoiding lifting heavy objects or intense straining.
For mild to moderate cases of prolapsed bladder, it is recommended to avoid lifting heavy objects or straining as well as practicing Kegel exercises to strengthen the pelvic floor muscles.
For more serious cases in the choice of treatment, factors such as: age, general health and severity of the prolapsed bladder are taken into account.
1. Ring Pessary
A pessary is a device made of plastic, silicone or rubber that is placed in the vagina to hold the bladder in place. The pessary should be removed and cleaned periodically to prevent infection (depending on the pessary, it is removed by the doctor or the patient).
2. Estrogen replacement therapy
It helps strengthen and maintain the tone of the muscles in the vagina. Women's bodies no longer create as much estrogen naturally after menopause and as a consequence the muscles of the vagina may weaken. Estrogen can be taken orally (pills) or topically (in the form of a patch or cream). Topically applied cream has a strong effect and presents lower risks compared to oral therapy.
The prolapse of the small intestine, also called enterococci, occurs when the small intestine descends into the lower pelvic cavity and pushes into the upper part of the vagina creating a bulge.
Childbirth, aging and other processes that put pressure on the pelvic floor can weaken the muscles and ligaments that support the pelvic organs, facilitating the prolapse of the small intestine.
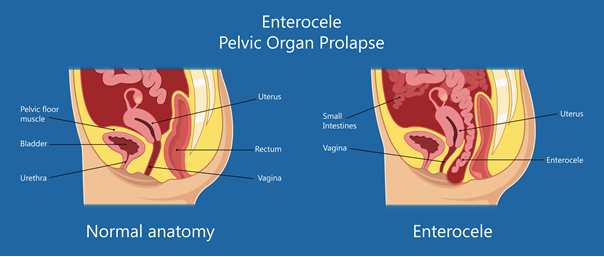
Most often the prolapse of the small intestine is asymptomatic. Only in severe cases the following may appear:
➢ Feeling of heaviness in the pelvis that eases with sleep
➢ Sensation of pelvic pressure or pain
➢ low back pain that improves with rest
➢ Soft swelling (tissue) in the vagina
➢ Vaginal discomfort and painful sexual intercourse (dyspareunia)
Many women with small intestine prolapse also show prolapse of other pelvic organs, such as the bladder, uterus or rectum.
Conditions and activities that can cause or contribute to the prolapse of the small intestine include:
➢ Pregnancy and childbirth
➢ Chronic constipation or bowel straining movements
➢ Chronic cough
➢ Repeated lifting of weights
➢ Overweight or obesity
➢ Pregnancy and the natural birth of one or more children contribute to the weakening of the pelvic floor support structures increasing the risk of prolapse.
➢ Age: the prolapse of the small intestine but also other types of pelvic organ prolapse appear more often with aging because as time goes by, muscle mass and strength are lost, generally affected being the pelvic floor muscles.
➢ Pelvic surgery: removal of the uterus (hysterectomy) or surgical procedures to treat urinary incontinence may increase the risk of developing small intestine prolapse.
➢ Increased abdominal pressure: excess body weight can increase pressure inside the abdomen which increases the risk of developing prolapse of the small intestine. Other factors that increase pressure include ongoing (chronic) coughing and straining during bowel movements.
➢ Chronic cough is associated with the development of prolapse because it increases abdominal pressure.
In order to prevent the prolapse of the small intestine, insist on maintaining the body weight within normal limits, on preventing constipation, on treating chronic cough and avoiding lifting heavy objects.
Prolapse of the small intestine usually does not need treatment if the symptoms do not bother. In this situation, only simple self-care measures are required, such as performing Kegel exercises to strengthen the pelvic floor muscles, avoiding lifting heavy objects and avoiding constipation.
When the symptoms become troublesome the following therapeutic options exist:
1.Ring Pessary
A silicone, plastic or rubber device will be inserted into the vagina to support the bulging tissue. The device is periodically removed for cleaning.
2.Surgery
The surgeon may perform surgery to repair the prolapse, through the vagina or abdomen, with or without robotic assistance. During the procedure, the surgeon moves the prolapsed small intestine back to its place and squeezes the weakened tissue of the pelvic floor. Sometimes small portions of special mesh can be used to help support weakened tissues

I always follow professional workflow and provide you the best service with reliable costs.

Rheumatoid arthritis that affects the shoulder region is a progressive disorder that leads to pain, loss of range ...
Although pregnancy seems like the perfect time for "laziness", fatigue can be felt more than usual and the back may ...
The hands are the two extremities, provided with fingers, of the upper limbs, and represent the main organ ...
