RADIUS AND ULNA FRACTURE
The skeleton of the forearm consists of two long bones, radius and ulna, which form the radioulnar joint and which are ...
Lumbar radiculopathy is a condition in which the pain, localized in the lower back, caused by a compressed nerve somewhere at the lumbar level, also radiates to the buttock area, in the back of the thigh and in the leg. In addition to pain, radiculopathy also causes numbness, weakness or tingling along the compressed nerve. Irradiated pain in the area behind the lower limb is often caused by pinching or compression of the sciatic nerve, while irradiated pain in front of the lower limb is usually caused by pinching or compression of the femoral nerve.
The disease can occur anywhere in the spine, but most commonly it occurs in the cervical or lumbar area, with irradiation of pain in the upper or lower limbs.
Pain caused by pinching or compressing the nerve is an intense pain.
Long-lasting positions, such as prolonged sitting or excessive extension (arching) can cause or accentuate pain, but there are also pain-relieving positions, called antalgic positions (sitting on your back or on one side with your knees bent towards the chest).
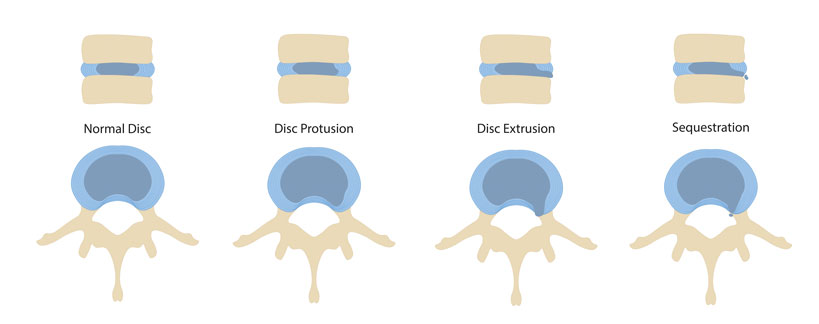
The main cause that compresses or pinches the nerve is a disc prolapse, a situation in which the intervertebral disc "slides" back compressing the nerve.
The disc can also swell and press on a nerve root causing numbness and pain on the innervation route of that nerve. The best example is the sciatic nerve that originates at the level of the lumbar vertebra L4 and crosses the entire lower limb, from its upper part to the plantar face of the foot.
Other factors that can also cause nerve compression are:
➢ Spondylolisthesis - when one of the vertebrae slips out of its place on the vertebra beneath it, which leads to the instability of the spine and can also put pressure on a nerve, causing the pain to be irradiated down on the lower limb.
➢ Spondylosis - a degenerative condition that manifests by an abnormal wear of the spine. The disease has a slow evolution and increases with age and the process of vertebral degeneration is the result of wear of the spine.
The spine consists of a number of 33 -34 small bones, called vertebrae. Superiorly, the first 24 vertebrae at the cervical, thoracic and lumbar level are articulated and separated from each other by the intervertebral discs and inferiorly, at the level of the sacral areas there are 5 welded vertebrae and at the level of the coccyx, bone located at the base of the spine, there are 4-5 joined vertebrae. The vertebrae are connected to each other, thus creating the vertebral canal in which the spinal marrow is housed and protected. The spine has 4 physiological curvatures: cervical, thoracic, lumbar and sacral. These curvatures increase the strength and elasticity of the spine, maintaining the normal position of the body.
The lumbar spine, consisting of 5 vertebrae, provides support for approximately the entire body weight.
Ligaments, nerves, muscles and intervertebral discs are additional components of the spine.
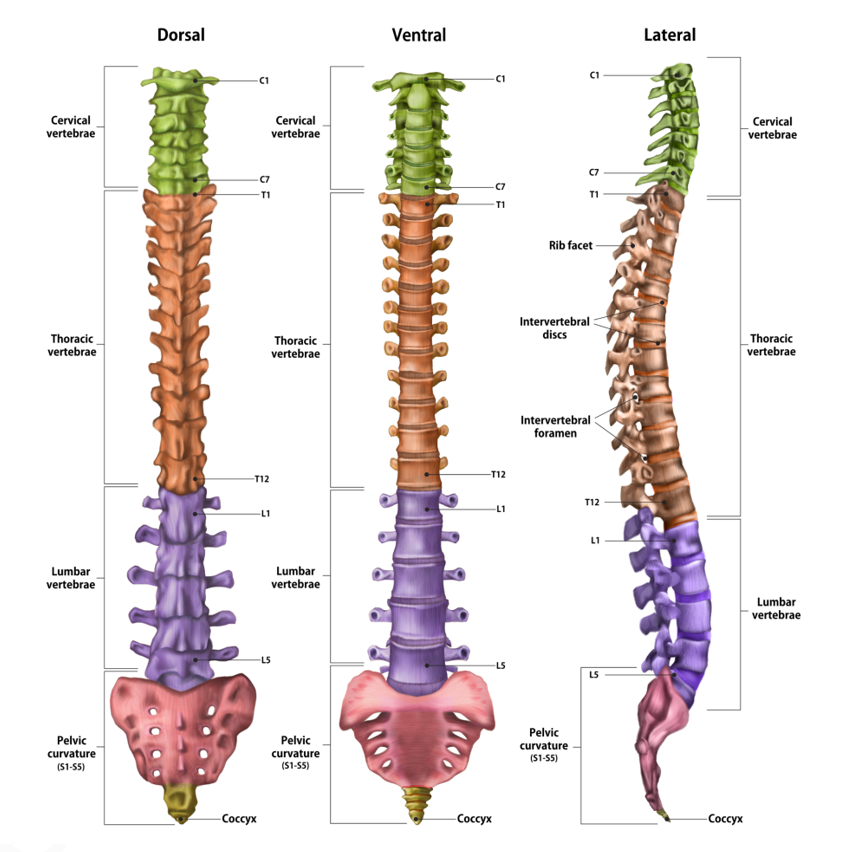
These are structures of fibrocartilaginous nature, placed between two vertebrae. They are essential for the movement of the spine and act as a ligament, tying a vertebra to the next, but they especially have a role in the absorption of shocks significantly diminishing the impact between the vertebrae. The discs are round and flat, with a thickness between 9-11 mm and consist of two components, a fibrous ring and a pulpy nucleus. The lumbar intervertebral discs are most in demand, because the greatest pressure acts on them.
They come from the spinal cord and come out through the holes of the vertebrae known as the vertebral foramen (in a normal vertebrae, the vertebral foramen is the hole or opening formed by the anterior segment of the vertebra, called the vertebral body and its posterior part, the vertebral arch).
When an intervertebral disc slips between the vertebrae, the nerve can become compressed in the place where the foramen exits.
Anti-inflammatory drugs reduce pain and inflammation in the affected area. As the inflammation decreases, the pain will also diminish. However, drug treatment is recommended for short periods of time, 10-14 days maximum.
If the pain and inflammation persist, a steroid and anesthetic drug can be injected between the vertebrae, at the level of the nerve involved. This helps to quickly reduce irritation and inflammation of the nerve. But it is a delicate procedure that is done either guided, under X-ray or ultrasound or by an experienced anesthesiologist.
It has an essential role in pain management and in reducing pressure on the compressed/pinched nerve. Initially, perform programs of exercises and positions that aim at:
➢ reducing pain
➢ improving mobility
➢ reducing pressure on nerve roots
As the exercises progress, the pain will alleviate and the recovery program can begin aiming at:
➢ increasing stability, more precisely the ability to control the position and movement in the lumbar area (which includes the abdomen - lower back - pelvic muscles).
➢ toning the back muscles, important both for strengthening as well as for the prevention of relapses or other injuries.
It’s indicated if the symptoms do not improve significantly with the help of conservative treatment (the therapeutic measures listed above). The goal of surgery is to alleviate compression of the affected nerve. After surgery, it is recommended to start the recovery program through physical therapy.
The treatment can last somewhere between 6 weeks, up to three months.
➢ Maintaining an adequate body weight helps alleviate any unjustified pressure in the lumbar area
➢ Avoid activities that affect the lumbar area, such as those that involve bending or tilting of the body excessively forward, as well as excessive arching
➢ Avoid lifting and carrying heavy weights
➢ Hold an adequate posture as much as possible, straight, to alleviate the pressure on the intervertebral discs
➢ Regular movement strengthens the paravertebral, abdominal and buttock muscles, thus providing a good support to the spine. A well-developed musculature helps prevent the appearance of the condition.

I always follow professional workflow and provide you the best service with reliable costs.

The skeleton of the forearm consists of two long bones, radius and ulna, which form the radioulnar joint and which are ...
Coxarthrosis is a condition that manifests itself with wear or degeneration of the hip joint. Similar to other joints that ...
Pelvic pain is localized in the lower abdomen and pelvis and can manifest itself as a symptom of diseases of the ...
